New Study Identifies Differential Outcomes in De Novo and Recurrent Metastatic Breast Cancer
NEW YORK, Oct 27, 2017 /PRNewswire/ — A retrospective analysis, reported in the journal Breast Cancer Research and Treatment, of more than 8,189 women with invasive breast cancer and 1,158 women diagnosed with metastatic breast cancer (MBC) between 1990 and 2010 identified differences in tumor characteristics and survival due to breast cancer in women diagnosed with de novo stage IV breast cancer (dnMBC) compared to those whose metastasis was the result of recurrent stage I-III disease (rMBC).
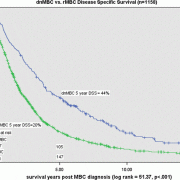
The study authors found that women with dnMBC had a five-year survival rate of 44 percent compared to 20 percent of women with rMBC. Over the 20-year period dnMBC five-year survival improved by 27 percent, from 28 percent to 55 percent, but rMBC survival decreased over time.
In other words, while incidence of dnMBC remained stable and five-year survival in this group improved over time, incidence of rMBC declined over the same period but survival time in this group decreased. This trend for rMBCcorresponded to a decrease in HER2-positive tumors and an increase of triple negative tumors. Across the entire cohort, worse survival was associated with hormone receptor-negative status, rMBC, having more than one site of metastasis, a dominant metastatic site of the liver, lung or brain, and age (over 70).
“We lump de novo and recurrent MBC in the same category with very little understanding of the differences in outcomes these patients may experience, and that’s a significant gap in our understanding of MBC,” explained study lead author Judith Malmgren, PhD. “In the absence of national data, we undertook this important and needed analysis of data from a local cancer breast registry of 12,000 primary breast cancers with robust longitudinal follow up.”
Summarizing the study findings, co-author Dr. Henry Kaplan noted three major take-aways:
- First, it is imperative that we track the course of metastatic breast cancer and the impacts of treatments. The Swedish Breast Cancer Registry enabled us to conduct this initial study, but we need to do this on a much larger scale.
- Second, in spite of the successes of early detection and improved preoperative and adjuvant treatments in reducing incidence of metastatic disease, this study points to the need for more effective treatment for those who do develop metastasis despite these treatments.
- Third, the finding that dnMBC behaves differently with regard to treatment response than rMBC requires further study to determine whether these patients truly have different types of disease from the start, or whether this is a manifestation of the development of resistance to initial therapy.
Recurrent breast cancers are not tracked in the national SEER or CDC databases, making it difficult to study the differences in tumor characteristics or patient outcomes between these two patient groups, whose tumors may very likely differ in biology and response to treatment.
Investigators from the Swedish Cancer Institute and the Metastatic Breast Cancer Alliance analyzed the cohort data including tumor histology, biomarkers, and five-year disease-specific survival in a retrospective breast cancer registry cohort of patients diagnosed with invasive breast cancer between 1990 and 2010 with follow up through 2015. The registry includes detailed information on diagnosis, stage of disease, tumor pathology, biomarkers, treatment and cause-specific death, as well as prospectively collected information on disease status including recurrence and death.
The analysis included 8,189 women, 1,158 with MBC (247 dnMBC and 911 rMBC) and covered intervals of time (1990-1998, 1999-2004, 2005-2010) to coincide with changes to systemic therapy for invasive and metastatic breast cancer, such as hormone therapy, HER2-directed therapies, taxanes and the use of neoadjuvant (pre-surgical) therapy.
This study is a unique comparison of survival and tumor characteristics between de novo and recurrent MBC in a robust cohort over two and half decades. Meticulous patient follow-up facilitated by a dedicated breast cancer registry prospectively tracking recurrence and treatment was essential to the study.
“We must not leave these MBC patients with hard to treat cancers behind. It is critical that we now focus intense research efforts on extending and saving these lives” said advocate and co-author, Musa Mayer.
Dr. Malmgren would like to recognize the unique research collaboration between patient advocates, the scientific and clinical community in tackling the problem of MBC that has been powered by support of the community intended to benefit from the research.
Study authors and affiliations:
Judith Malmgren, PhD affiliate assistant professor of epidemiology, University of Washington School of Public Health and President of HealthStat Consulting, Inc., Seattle WA
Musa Mayer, Metastatic Breast Cancer Alliance
Mary K. Atwood, Swedish Breast Registry
Henry Kaplan, MD, Chief Medical Oncology Breast Cancer Service of the Swedish Cancer Institute and clinical professor of Medicine, University of Washington
The study was supported Kaplan Cancer Research Fund and the Metastatic Breast Cancer Alliance.
About the Swedish Cancer Institute
The Swedish Cancer Institute (SCI) opened in 1932 as the first dedicated cancer-care center west of the Mississippi. Now in its 75th year, it is the largest and most comprehensive cancer treatment program in the Pacific Northwest. A true multidisciplinary program, SCI offers a wide range of advanced cancer-treatment options in chemotherapy, radiation therapy and surgery – backed by extensive diagnostic capabilities, patient education and support-group services. SCI’s clinical-research arm encompasses industry-sponsored and cooperative group therapeutic trials, cancer screening and prevention trials, and investigator-initiated trials. Breast-cancer screening and diagnostics are available through the Swedish Breast Care Centers and mobile mammography units. For more information, visit www.swedish.org
About Swedish
Founded in 1910, Swedish is the largest non-profit health provider in the Greater Seattle area. It is comprised of five hospital campuses (First Hill, Cherry Hill, Ballard, Edmonds and Issaquah); ambulatory care centers in Redmond and Mill Creek; and a network of more than 183 primary care and specialty-care clinics located throughout the Greater Puget Sound area. In addition to general medical and surgical care including robotic-assisted surgery, Swedish is known as a regional referral center, providing specialized treatment in areas such as cardiovascular care, cancer care, neuroscience, orthopedics, high-risk obstetrics, pediatric specialties, organ transplantation and clinical research. In 2016, Swedish provided more than $247 million in community benefit programs, including $21.6 million in free and discounted care in Western Washington. For more information, visit www.swedish.org
About the Kaplan Cancer Research Fund
The Kaplan Cancer Research Fund at Swedish was started in 1984 as a series of grants that Dr. Henry Kaplan had received while doing research related to experimental drug trials and has continued with similar funding as well as major philanthropic support. Research efforts have included work on appropriate use of mammography, outcomes of breast cancer treatments, effects of chemotherapy drugs on the development of hematologic malignancy, pharmacology of chemotherapy drugs, cancer genomics, and clinical drug trials.
About the MBC Alliance
The Metastatic Breast Cancer Alliance (MBCA) is a consortium made up of representatives from 32 nonprofit organizations and 11 pharmaceutical/biotech companies, along with 14 individual patient advocates – many of whom are living with MBC. The mission of the MBCA is to improve the lives of, and outcomes for, those living with metastatic breast cancer and their families through increasing awareness and education about the disease and advancing policy and strategic coordination of research funding, specifically focused on metastasis, that has the potential to extend life, enhance quality of life and ultimately to cure.
Media Contact:
Laurie Campbell
646-239-7872
lauriembcalliance@bcrfcure.org
SOURCE Metastatic Breast Cancer Alliance